With over 463 million adults living with diabetes globally and this number projected to rise to 700 million by 2045, the demand for skilled diabetes educators has never been higher. In the United States alone, more than 34 million people have diabetes, with an additional 88 million adults at risk due to prediabetes. This comprehensive guide reveals the hidden pathways and unspoken realities of becoming a diabetes educator. I’ll walk you through everything from the psychological skills you actually need to succeed, to the business side nobody talks about, plus the emerging opportunities that could shape your entire career trajectory.
Whether you’re a nurse looking to specialize or someone passionate about helping people manage chronic conditions, this is your roadmap to understanding what it really takes to thrive in diabetes education.
Table of Contents
- The Psychology Behind Effective Diabetes Education
- Understanding How Habits Actually Form in Diabetes Management
- Cultural Competency That Goes Beyond the Textbook
- The Business Reality of Diabetes Education
- Revenue Streams and Getting Paid
- Your Certification Strategy Decoded
- The Innovation Wave You Need to Ride
- AI and Personalized Patient Care
- Mastering Telehealth and Remote Monitoring
- Building Your Career and Finding Your Niche
- Specialization Opportunities That Pay
- Leadership Roles and Making Real Impact
TL;DR
- Successful diabetes educators master psychology and behavior change, not just medical facts
- The business side involves complex insurance navigation and understanding value-based care metrics
- CDCES certification requires strategic planning around the 1,000-hour experience requirement
- Technology integration is crucial, but you need to balance digital tools with human connection
- Cultural competency means understanding food as identity and addressing historical medical trauma
- Specialization in areas like pediatric or gestational diabetes creates competitive advantages
- Remote care skills became essential post-pandemic and require different communication strategies
- Professional involvement in organizations like AADE accelerates career advancement
The Psychology Behind Effective Diabetes Education
Most people think diabetes education is about teaching carb counting and insulin dosing. That’s barely scratching the surface. The educators who actually change lives understand that diabetes management happens in the brain first. You’re dealing with grief, fear, cultural identity, and deeply ingrained habits. I’ve seen brilliant clinicians fail because they focused on the medical stuff while ignoring the psychological landscape their patients were navigating.
Understanding the psychological foundations of diabetes education requires a deep appreciation for how educational achievements shape both patient and educator confidence. Many successful diabetes educators find that displaying their credentials professionally helps establish trust and credibility with patients from the very first consultation.
The CDCES credential becomes particularly important when patients are evaluating whether to trust your guidance. When someone walks into your office facing a life-altering diagnosis, they need to see evidence that you have the expertise to guide them through this journey. Your displayed certifications communicate competence before you even speak.
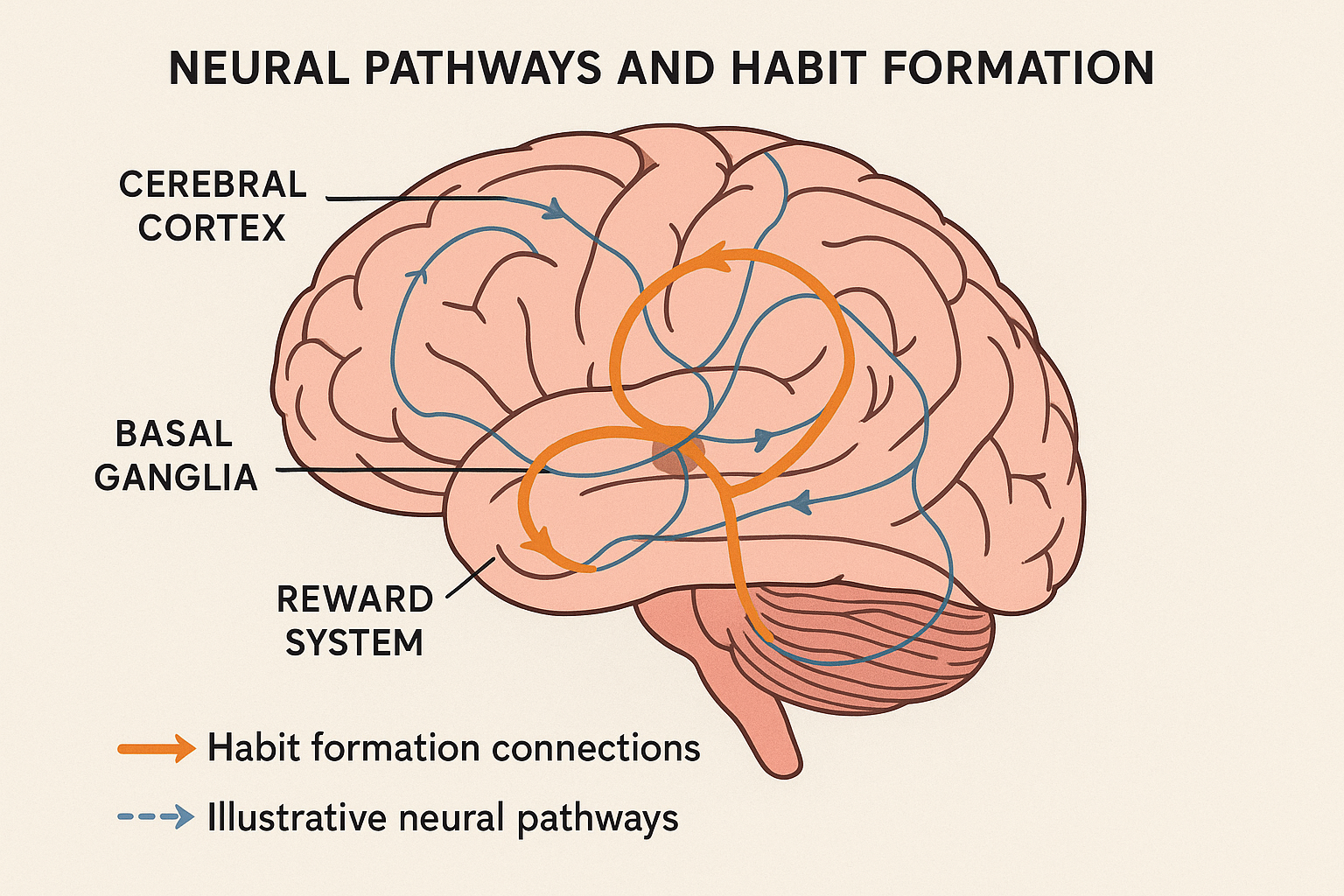
Understanding How Habits Actually Form in Diabetes Management
Your brain doesn’t care about your HbA1c goals – it cares about dopamine hits and cognitive shortcuts. When you understand how neural pathways actually work, you can design interventions that stick instead of fighting against human nature. This isn’t about willpower; it’s about working with the brain’s natural reward systems to make healthy behaviors feel automatic rather than forced.
Take Sarah, a 45-year-old teacher who consistently forgot to check her blood sugar before lunch. Instead of lecturing her about compliance, her CDCES educator helped her link glucose checking to her existing habit of setting her phone alarm for lunch break. Within two weeks, the glucose check became automatic because it piggybacked on an established neural pathway. The key was working with her brain’s existing patterns rather than fighting them.
The most effective CDCES professionals I know have learned to identify these existing behavioral anchors in their patients’ lives. They don’t try to create entirely new routines from scratch. Instead, they attach new diabetes management behaviors to things people already do consistently.
Leveraging Dopamine in Blood Sugar Monitoring
Every successful glucose reading triggers a tiny dopamine release, but most patients never learn to recognize or amplify this natural reward. I teach educators how to help patients identify these moments and build on them. It’s about celebrating the small wins and creating positive feedback loops that make monitoring feel rewarding rather than punitive.
When patients start associating their glucose meter with success instead of judgment, everything changes. The CDCES certification process actually covers this neurochemistry, but many educators don’t apply it practically. You need to help patients reframe their relationship with their monitoring devices.
Habit Formation Checklist for Diabetes Educators:
- ☐ Identify existing patient routines to anchor new behaviors
- ☐ Celebrate small wins to trigger dopamine release
- ☐ Use visual cues and reminders in patient’s environment
- ☐ Start with micro-habits (30-second actions)
- ☐ Track progress visually with charts or apps
- ☐ Address emotional barriers before behavioral ones
- ☐ Create if-then scenarios for challenging situations
Managing Cognitive Load in Patient Education
Your patients’ brains can only handle so much new information at once. I’ve watched educators overwhelm newly diagnosed patients with everything from carb ratios to exercise guidelines in a single session. The smart approach? Start with survival skills – recognizing and treating lows, basic meal planning, when to call for help.
Build complexity gradually as confidence grows. The CDCES curriculum emphasizes this staged approach, but implementing it requires discipline. You want to share everything you know immediately, but restraint serves your patients better.
| Education Phase | Focus Areas | Cognitive Load Level | Timeline |
|---|---|---|---|
| Survival Skills | Hypo/hyperglycemia recognition, emergency contacts | Low | Week 1-2 |
| Basic Management | Simple carb counting, medication timing | Medium | Week 3-6 |
| Advanced Skills | Insulin adjustments, exercise planning | High | Month 2+ |
| Lifestyle Integration | Social situations, travel planning | Variable | Ongoing |
Cultural Competency That Goes Beyond the Textbook
Real cultural competency isn’t about memorizing which ethnic groups prefer rice over bread. It’s about understanding how different communities view illness, the role of family in health decisions, and why some patients carry deep mistrust of medical institutions. You’ll encounter patients whose grandmother’s diabetes remedies conflict with your evidence-based recommendations, and you need skills to navigate these conversations with respect and effectiveness.
Recent research highlights the importance of culturally competent diabetes education. As diabetes educator and advocate Bridget Wood explains, “Black people and people of color are not a monolith – we’re all different. At the end of the day, we are coming in to get care and we trust these people with our lives. The expectation should be that we’re receiving care without judgment.”
The CDCES certification process touches on cultural competency, but real-world application requires ongoing learning and self-reflection. You’ll make mistakes. I certainly have. The key is staying humble and adjusting your approach based on patient feedback.
When Food Represents More Than Nutrition
Food isn’t just fuel for most of your patients – it’s identity, comfort, family connection, and cultural heritage all rolled into one. When you tell someone to eliminate their grandmother’s tamales or their family’s Sunday pasta tradition, you’re asking them to give up pieces of themselves. Effective educators learn to work within these food relationships rather than against them, finding ways to honor cultural significance while managing blood sugar.
Maria, a 52-year-old Mexican-American woman, was told to “cut out rice and beans” by her previous educator. She stopped attending appointments because these foods represented her connection to her late mother’s cooking. Her new CDCES educator took a different approach: they worked together to modify portion sizes, add fiber-rich vegetables, and time insulin doses around family meals. Maria’s HbA1c improved from 9.2% to 7.1% while maintaining her cultural food traditions.
This approach requires more time and creativity than generic meal planning, but the results speak for themselves. Your CDCES training will give you the clinical foundation, but cultural sensitivity comes from listening more than talking.
Addressing Historical Medical Trauma
Many communities carry generational wounds from medical experimentation, discrimination, and neglect. Your patients might walk into your office already expecting to be judged, dismissed, or treated as a number rather than a person. Building trust requires acknowledging these realities and proving through your actions that you’re different.
It’s not enough to be well-intentioned; you need to be actively anti-racist and culturally humble in your approach. The CDCES certification process includes some training on health disparities, but you’ll need to seek additional education to truly understand the communities you serve.
The Economics of Diabetes Management
Monthly diabetes supplies can cost over $500 for uninsured patients. You’ll become part social worker, part financial counselor as you help patients navigate insurance coverage, find patient assistance programs, and identify cost-effective alternatives. Understanding the economic barriers your patients face is crucial – you can’t educate someone who can’t afford to implement your recommendations.
The financial burden of diabetes management is staggering, with monthly supplies potentially costing over $500 for uninsured patients. This economic reality means diabetes educators must become skilled at helping patients navigate insurance coverage, find patient assistance programs, and identify cost-effective alternatives to ensure their recommendations are actually implementable.
The Technology Integration Challenge
Technology offers incredible opportunities for diabetes management, but it also creates new barriers. Not everyone has a smartphone, reliable internet, or the digital literacy to use continuous glucose monitors effectively. Modern diabetes educators need to be fluent in digital health tools while maintaining analog backup systems for underserved populations.
It’s about meeting patients where they are, not where you think they should be. Your CDCES training will cover the latest devices and apps, but you’ll need to develop assessment skills to determine what actually works for each individual patient.
Bridging the Digital Divide
Continuous glucose monitors and diabetes apps assume access to technology that many patients don’t have. You’ll need to assess each patient’s digital resources and literacy level, then develop parallel systems that work for everyone. Sometimes the most high-tech solution isn’t the most effective one for your specific patient population.
The CDCES curriculum includes technology training, but real-world implementation requires flexibility and creativity. You might find yourself teaching a 70-year-old grandmother how to use a smartphone app while simultaneously helping her adult children understand how to support her diabetes management.
Digital Assessment Checklist:
- ☐ Smartphone access and comfort level
- ☐ Internet reliability and data plan limitations
- ☐ Previous experience with health apps
- ☐ Vision/dexterity challenges with small screens
- ☐ Language preferences for digital interfaces
- ☐ Family support for technology troubleshooting
- ☐ Backup analog systems needed
The Business Reality of Diabetes Education
Nobody talks about the business side of diabetes education, but understanding it determines whether you’ll thrive or struggle in this field. Healthcare is a business, and diabetes education exists within complex webs of insurance reimbursement, value-based care metrics, and institutional priorities.
You need to know how you’ll get paid, what metrics matter to your employers, and how to position yourself for success within these systems. The CDCES certification opens doors, but business acumen keeps them open. I’ve seen talented educators struggle because they didn’t understand the financial realities of their practice settings.
Revenue Streams and Getting Paid
Diabetes education reimbursement is complicated. Different rules apply for individual versus group sessions, initial versus follow-up visits, and medical nutrition therapy versus diabetes self-management education and support (DSMES). Understanding these distinctions helps you maximize patient access while ensuring sustainable practice operations.
You’ll also need to become skilled at insurance navigation and appeals processes. This administrative work is part of patient advocacy – helping people access the education they need despite bureaucratic barriers. Your CDCES credential helps with reimbursement approval, but you still need to understand the system.
Mastering Insurance Navigation
Insurance companies have specific requirements for diabetes education coverage, and these rules change frequently. You’ll spend significant time on prior authorizations, appeals, and finding alternative funding sources when insurance denies coverage.
The CDCES certification gives you credibility with insurance companies, but you’ll still face denials and need to advocate for your patients. I keep a running list of successful appeal language and update it regularly based on what works with different insurers.
| Insurance Type | Coverage Requirements | Typical Limitations | Appeal Success Rate |
|---|---|---|---|
| Medicare | Physician referral required | 10 hours initial, 2 hours follow-up | 65% |
| Private Insurance | Varies by plan | 4-8 hours annually | 45% |
| Medicaid | State-specific rules | Often unlimited with authorization | 70% |
| Self-Pay | No restrictions | Cost barrier ($150-300/hour) | N/A |
Understanding Value-Based Care Metrics
Healthcare systems increasingly measure diabetes educators based on patient outcomes like HbA1c reduction, hospitalization rates, and medication adherence. These metrics affect your job security and advancement opportunities. Understanding what your employer values helps you align your practice with institutional goals while maintaining patient-centered care.
Your CDCES training covers outcome measurement, but you need to understand how these metrics translate into performance evaluations and compensation decisions. Some organizations tie bonuses directly to patient outcome improvements.
Your Certification Strategy Decoded
The CDCES (Certified Diabetes Care and Education Specialist) certification is your ticket to credibility and better job opportunities, but the path requires strategic planning. You need 1,000 hours of diabetes-related experience before you can even sit for the exam, and the test itself requires specific preparation strategies.
This isn’t just about studying harder; it’s about studying smarter. The path to CDCES certification often requires documenting extensive educational and professional achievements. Many candidates find themselves needing to replace lost diplomas or obtain copies of their transcripts when applying for certification, making it essential to have reliable access to your educational documentation.
The CDCES certification requires a minimum of 1,000 hours of diabetes care and education experience within the 5 years prior to application, with at least 200 hours accrued in the most recent year. Additionally, candidates need 2 years of professional practice experience in their discipline, though this can be reduced to 1 year with a master’s degree or higher in a health-related field.
CBDCE Exam Preparation That Actually Works
The Certification Board for Diabetes Care and Education (CBDCE) exam tests more than textbook knowledge – it requires you to think like the test writers. Successful candidates learn the exam format, practice with realistic questions, and develop test-taking strategies specific to this certification.
I recommend starting your exam prep at least six months before your planned test date. The CBDCE exam covers clinical knowledge, but it also tests your ability to apply that knowledge in realistic scenarios. You need to understand not just what to do, but why certain approaches work better than others.
The CBDCE uses a specific question format that can trip up even experienced clinicians. Practice exams help you get comfortable with their style and timing requirements. Many candidates underestimate the time management aspect of the CBDCE exam.
CDCES Exam Preparation Timeline:
- ☐ 6 months before: Register for exam, order study materials
- ☐ 5 months before: Begin systematic content review
- ☐ 4 months before: Join study group or online community
- ☐ 3 months before: Start practice exams weekly
- ☐ 2 months before: Identify weak areas, focus review
- ☐ 1 month before: Final review, practice time management
- ☐ 1 week before: Light review, rest, prepare mentally
Accumulating Your Required Experience Hours
Those 1,000 hours of diabetes-related experience can come from clinical practice, research, program development, or community education. Strategic planning helps you maximize qualifying experience while building skills that make you more marketable. Document everything – you’ll need detailed records for your CBDCE application.
Jennifer, an RN working in a family practice clinic, strategically built her 1,000 hours over 18 months. She volunteered at diabetes support groups (150 hours), attended diabetes conferences (40 hours), participated in a workplace wellness program (200 hours), and gradually took on more diabetes patients in her clinical role (610 hours). By documenting everything meticulously, she had her required hours plus diverse experience that made her attractive to employers.
The CBDCE is strict about documentation requirements. Keep detailed logs of your activities, including dates, hours, and specific diabetes-related tasks. Vague descriptions won’t pass their review process.
The Innovation Wave You Need to Ride
Diabetes education is evolving rapidly with artificial intelligence, personalized medicine, and novel delivery methods. The educators who position themselves at the intersection of technology and human connection will have the most opportunities and impact.
This isn’t about replacing human expertise with machines; it’s about using technology to enhance your ability to provide personalized, effective education. Your CDCES training will introduce you to current technologies, but staying current requires ongoing learning and adaptation.
The field rewards early adopters who can demonstrate measurable improvements in patient outcomes through technology integration. However, you need to balance innovation with accessibility – not every patient can or wants to use the latest digital tools.
AI and Personalized Patient Care
Machine learning algorithms can analyze patterns in glucose data, lifestyle factors, and behavioral responses to create highly personalized education plans. Your role becomes interpreting these insights and translating them into human-centered interventions. AI can identify which patients are at risk for complications, but you provide the emotional support and practical guidance they need to change their behaviors.
The CDCES curriculum is starting to include AI applications, but the technology evolves faster than certification programs can keep up. You’ll need to stay current through continuing education and professional development opportunities.
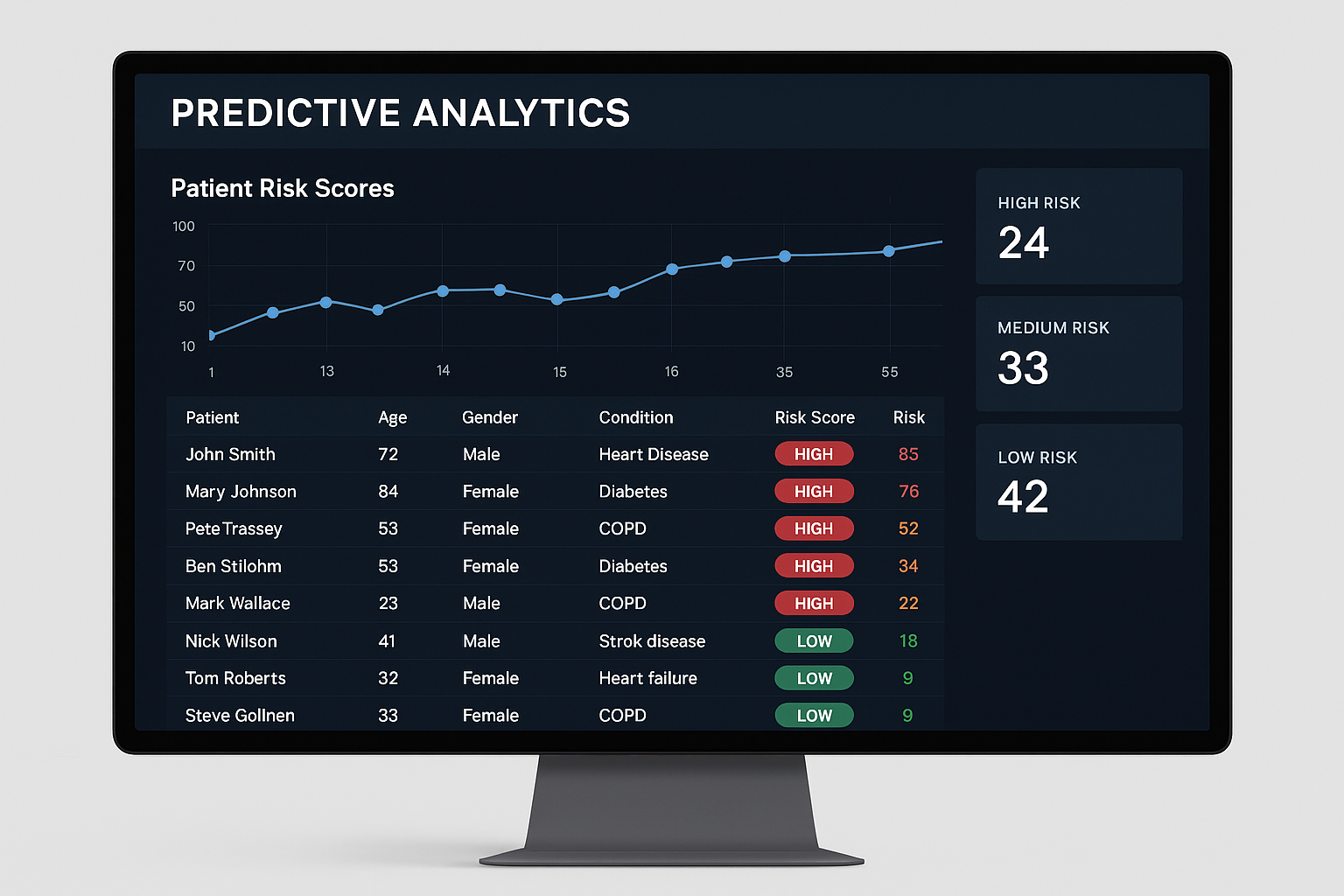
Using Predictive Analytics for Proactive Care
Advanced systems can predict which patients are likely to have poor outcomes or stop following their management plans. This allows you to intervene before problems become crises. Instead of waiting for patients to miss appointments or show up in the emergency room, you can reach out proactively with additional support and resources.
The CDCES training covers risk assessment, but predictive analytics takes this to another level. You can identify patterns that human observation might miss and adjust your interventions accordingly.
Mastering Telehealth and Remote Monitoring
The pandemic accelerated adoption of remote diabetes education, and these skills are now essential rather than optional. Effective virtual care requires different communication strategies, visual aids, and follow-up approaches than in-person education.
You’ll also need to become skilled at troubleshooting technical problems with glucose meters and other devices through video calls. Healthcare systems are rapidly expanding their diabetes education programs to meet growing demand. As UAB expert Mariah Stewart, RDN, explains, “A CDCES offers much more to patients than an educational flyer. Patients receive ongoing support and resources to make the difficult lifestyle changes needed to control diabetes.” The UAB Medicine Outpatient Diabetes and Nutrition Education Clinic now offers American Diabetes Association-accredited programs covering everything from nutrition to stress management.
The CDCES certification now includes telehealth competencies, but mastering virtual care requires practice and ongoing skill development. You need to create the same level of connection and trust through a screen that you would in person.
Building Connection Through Screens
Creating emotional connection and trust through video calls requires intentional strategies. You need to master eye contact with the camera (not the screen), use body language effectively in a small video window, and create intimate conversational spaces despite physical distance.
The technical quality of your setup affects your professional credibility and patient engagement. Poor audio or video quality can undermine even the best clinical content. Your CDCES training might not cover these technical aspects, but they’re crucial for successful virtual practice.
Telehealth Setup Checklist:
- ☐ High-quality webcam at eye level
- ☐ Professional lighting (ring light or window light)
- ☐ Noise-canceling headset or microphone
- ☐ Stable internet connection (ethernet preferred)
- ☐ Neutral, professional background
- ☐ Backup communication method (phone)
- ☐ Screen sharing capabilities for educational materials
- ☐ HIPAA-compliant video platform
Remote Device Troubleshooting Skills
You’ll frequently need to diagnose problems with glucose meters, insulin pens, and continuous glucose monitors through verbal description and video demonstration. This requires patience, clear communication skills, and familiarity with common technical issues across different device brands.
Sometimes you’re part educator, part tech support. The CDCES curriculum covers device operation, but remote troubleshooting is a specialized skill that requires additional training and experience.
Building Your Career and Finding Your Niche
The diabetes education field offers diverse career paths beyond traditional clinical roles. You can specialize in specific populations, move into program development or research, advocate for policy changes, or even start your own practice.
Strategic career planning helps you maximize both your impact on patients and your earning potential. The key is identifying your strengths and interests, then positioning yourself in growing market segments. Your CDCES certification opens doors, but specialization creates competitive advantages.
Specialization Opportunities That Pay
As diabetes education matures, subspecialties are emerging that command higher salaries and offer more interesting work. Pediatric diabetes, gestational diabetes, technology integration, and population health management all represent growing niches.
Early specialization can create competitive advantages and open doors to leadership opportunities. Specialized diabetes education roles often require additional certifications and credentials beyond basic nursing or healthcare degrees. Many professionals find that understanding the different types of degrees and business certifications helps them strategically plan their educational pathway for maximum career impact.
The CDCES certification provides a foundation, but specialization requires additional training and experience in your chosen area. Market demand varies by region and healthcare system, so research opportunities in your area before committing to a specialty path.
Pediatric Diabetes Education Expertise
Working with children and adolescents requires specialized skills in developmental psychology, family dynamics, and age-appropriate communication. This specialization is increasingly valuable as Type 2 diabetes rates rise in youth populations.
You’ll work closely with schools, families, and pediatric endocrinology practices, often becoming a central coordinator for complex care teams. The CDCES training covers pediatric considerations, but specializing requires additional education in child development and family systems.
Gestational Diabetes Management
The temporary nature of gestational diabetes creates unique educational challenges and opportunities. You need to help women make significant lifestyle changes quickly while managing the emotional complexity of pregnancy.
Specialists in this area often work closely with obstetric practices and develop expertise in rapid behavior change techniques that can be applied to other populations. The CDCES curriculum includes gestational diabetes, but specialization requires understanding pregnancy physiology and maternal-fetal medicine.
Leadership Roles and Making Real Impact
Experienced educators often transition into roles that shape policy, develop programs, and advocate for patient access to care. These positions require skills in project management, public speaking, and stakeholder engagement.
Leadership roles offer the opportunity to influence practice standards and improve care for entire populations rather than individual patients. Your CDCES credential provides credibility for these positions, but leadership skills require separate development.
Getting Involved with Professional Organizations
Active participation in organizations like the American Association of Diabetes Educators (now the Association of Diabetes Care & Education Specialists) provides networking opportunities, leadership development, and influence over practice standards.
Strategic involvement can accelerate your career advancement and give you a voice in shaping the future of diabetes education. The CDCES certification connects you to this professional community, but meaningful involvement requires time and commitment beyond maintaining your credential.
When you’re building your diabetes education career, you might find yourself needing backup documentation of your educational achievements. Whether you’re applying for CDCES certification, seeking employment, or presenting qualifications to healthcare institutions, having reliable access to your credentials is crucial.
ValidGrad understands that original diplomas and transcripts can be lost, damaged, or delayed when you need them most. Our professional document replacement service ensures you always have access to high-quality replicas of your educational achievements – particularly valuable for diabetes educators who often need to provide documentation to multiple employers, certification boards, and continuing education providers.
Final Thoughts
Becoming a diabetes educator isn’t just about getting certified and finding a job – it’s about positioning yourself for a career that evolves with healthcare innovation while maintaining the human connection that makes real change possible. The field rewards those who understand both the science and the art of behavior change, who can navigate complex business realities while advocating for their patients, and who embrace technology without losing sight of individual needs and cultural contexts.
The diabetes education field is expanding rapidly, driven by rising diabetes prevalence and growing recognition that education prevents costly complications. Your success depends on understanding the psychological aspects of chronic disease management, mastering the business dynamics of healthcare reimbursement, and positioning yourself at the forefront of technological innovation.
Remember that every patient you work with is dealing with more than just blood sugar numbers. They’re navigating fear, grief, cultural expectations, and economic constraints while trying to make sense of a complex medical condition. Your role extends far beyond teaching carb counting – you’re helping people reclaim control over their lives and health.
The most successful diabetes educators I know are those who never stop learning, who advocate fiercely for their patients, and who find ways to blend evidence-based practice with genuine human compassion. This career path offers the opportunity to make a profound difference in people’s lives while building expertise in one of healthcare’s most critical areas.
Your CDCES certification is just the beginning. The real work happens in those moments when you help someone understand that diabetes doesn’t define them – it’s just something they manage while living their full, rich lives.